Exploring American Primary Care: Southcentral Foundation
As a medical student and a public health professional, I see the current American healthcare landscape through a lens of concerned optimism. We, as a nation, have been taught that our perspectives on healthcare are vastly divided. Yet, I believe we have more in common regarding what we want from health care delivery than we currently understand. Through a series of interviews, I seek to study these common values and further highlight creative approaches to primary care that exist within the United States.
Over the past year, I have been reaching out to innovative designers within primary care to learn more about their motivation, their failures, their successes, and most importantly the health outcomes of their patients. As a student of health system design, it has been a long-time dream of mine to visit Southcentral Foundation (SCF) in Alaska. Through serendipity, the opportunity arose to spend two weeks studying with Family Medicine providers at one of SCF’s main clinics in Anchorage. My hope was to use this time to develop a deeper understanding about this organization’s unique approach to delivering primary care services.
In addition to providing high quality healthcare, Southcentral Foundation offers a rich environment for the cultivation of innovative ideas in primary care design. This past April when I placed one foot on the snow-covered ground of their campus, I felt like I had finally arrived in an environment I had long been searching for.
From the architecture inspired by Alaska Native cultures, to a traditional herbal garden which serves as a symbol for the organization's respect for traditional healing, this clinic speaks to the community. As one walks into the lobby of SCF’s primary care clinic, it is hard to miss the massive wooden beams that surround the open atrium. The beams provide the illusion that one is walking inside the hull of a ship, or perhaps through a forest. What is effectively communicated, without words, is a powerful sense that this is a safe place for health and healing. The space is intentionally designed to reflect the values of the Alaska Native population that it serves. In fact, Southcentral Foundation as a whole has been created to reflect these values.
Photo Source: NBBJ
Dr. Steve Tierney, Medical Director of Quality Improvement and Chief Medical Informatics Officer at SCF, extended an offer to spend a day with him to better understand the approach that the organization takes to healthcare. One afternoon, he invited me to meet him in his office. I arrived to find a massive room, filled with others working diligently, and eventually found him at his desk amidst this open-concept shared office space.
As I sat down across from his desk, he offered me tea. I politely refused, since as a medical student I am not accustomed to my attending physicians going out of their way to make me tea, nor would I ever imagine imposing this request on a busy doctor. But Dr. Tierney pressed further, “Are you sure?” he asked, sagely reminding me that every once and awhile it’s good to take a pause for reflection, and tea helps facilitate this. With a soothing Earl Grey in hand, we began to discuss the core values of Southcentral Foundation.
In the early part of our conversation, I asked him what he believed patients value from their primary care experience at SCF. He put his hand up, and stopped me, correcting my use of the word patients. At Southcentral Foundation one of the core values is to not use the word “patients,” but instead refer to people receiving health care as “customer owners.” As members of this aggregate tribal community, all individuals are, in fact, partial owners of the organization.
This small detail represents a powerful shift in the power dynamics inherent to the patient-provider relationship. When one steps back to recognize that a patient is actually an individual paying for service it is obvious that they could be classified as a customer. This changes the interaction between a provider with many years of academic training and someone who does not have the same knowledge of medicine and healthcare.
“When we reframe our perception of patients as customers of a healthcare system, it encourages more intentional choice in the conversation regarding what kind of services are given or provided.”
Additionally, when patients are viewed as customers, it gives people the opportunity to feel like they have more autonomy in what they do with information. Southcentral Foundation is able to take this concept one step further. Their board is comprised of customer-owners and that is also intentional. In our traditional American healthcare system (where people ideally have insurance), patients pay a third party insurance company to somehow pay for health services rendered. This separates the person receiving healthcare from understanding the value placed on the services. When we reframe our perception of patients as customers of a healthcare system, it encourages more intentional choice in the conversation regarding what kind of services are given or provided.
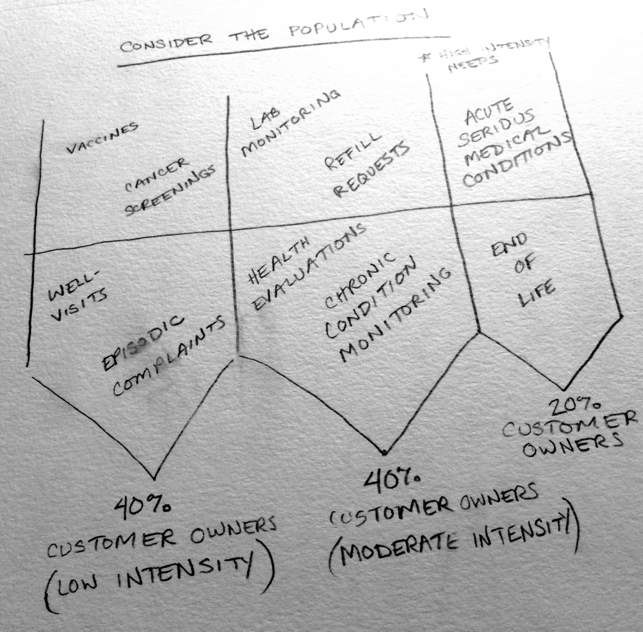
When I asked for an example of how the organization thinks differently about utilization of resources, Dr. Tierney stood up and walked to a nearby white board (whiteboards were everywhere in this shared work space to support visual exchanges, exactly like the conversation we were having in that moment). He grabbed a marker and started drawing a graph on the board. He began, “consider the population” he said as he drew out a graph of the customer owner population on the board. This graph was divided by percentages of customer owners who utilize the health care system with low intensity, moderate intensity, and high intensity. He was encouraging me to think more critically about how we use our resources for each of these groups. Because, in fact, the way resources are used for each of these groups doesn’t necessarily need to be the same. For example, 40% of customer owners use healthcare with low intensity, meaning that they are coming in for vaccines, cancer screenings, well visits, or some kind of episodic complaint. These encounters are relatively simple and quick to address adequately. These patients do not necessarily need that much time, or even medical knowledge, to take care of them appropriately.
Next he said, “let’s consider the following portion of the population.” About 40% of customer owners utilize the system with moderate intensity, meaning that they have some labs that need to monitored, medication refills that need to be thoughtfully considered, or chronic conditions that require some sort of monitoring. These visits are more complex, but they are also routine. There is a systematic approach to dealing with these complaints. So they need a different approach to care than the first 40%.
That leaves us with 20% of the population. These customer-owners are utilizing the system with high intensity. They have acute, serious medical conditions. They may be in and out of the hospital, or may be experiencing an end of life situation. These individuals will inevitably take a lot of time and energy on the part of the medical staff. His description is actually a perfect demonstration of the classic 80-20 rule, where 20% percent of any given population requires 80% of the resources to achieve a common goal, in this case health.
Another interesting approach that Dr. Tierney mentioned was SCF’s use of the team model. Each SCF integrated care team consists of a provider (PA, NP, MD, or DO), paired with a nurse (an RN), as well as a certified medical assistant and case management support, all working literally side-by-side to achieve their common goals. Several teams share an office space to allow for easy exchange of questions and ideas between the groups. Within that shared environment, there are behavioral health professionals that are accessible for helping with mental health needs.
Additionally, there are pharmacists within this shared open office space, to address pharmaceutical questions as they arise. This is something I have never seen outside of the Emergency Department. Several times, I watched in awe as my preceptors walked over to a pharmacist, just a few feet from their desk, to ask intricate questions about the role of pharmaceuticals in their specific clinical case at hand. I have no doubt that this thorough level of communication decreases prescription errors.
Towards the end of our conversation, I asked Dr. Tierney what he saw as positive and negative attributes of the American healthcare system. He believed that the most positive aspects of our system were the extensive opportunities for disruptive innovation. Dr. Tierney then explained his three-part answer regarding the negative attributes of the American healthcare system. First, insurance. The insurance we have doesn’t easily cross state lines. It is very confusing to compare insurance policies, even despite the online marketplaces that we have. Ideally the best product is the one that wins in a free market, but without easy comparison, this level of competition is not possible. Additionally, price transparency is an issue. There is very little information available regarding the costs of services within American healthcare. And, to add insult to injury, there isn’t even price consistency for the same quality service delivered by different organizations. Finally, Dr. Tierney suggested that one substantial opportunity for improvement was our current reliance on American pharmaceuticals. He felt that foreign manufactured pharmaceuticals, especially with efforts in place to demonstrate safety and quality, served as a unique opportunity for innovation and progress. The way it is now, the American pharmaceutical organizations have tight control over prices and there is limited competition. Dr. Tierney shared his belief that the ability to outsource our pharmaceuticals to well-respected foreign manufacturing companies is something that we should all consider more seriously.
“It is ok to think differently about the status quo, about what can be done to not only to make healthcare better, but to make it something entirely new.”
Dr. Tierney’s thoughts on healthcare were inspiring, and I admire his willingness to change the rules of engagement. Unfortunately, within the current system, we are unlikely to get far in improving our system of healthcare unless these rules do change. For me, the beauty of being able to study at Southcentral Foundation was the opportunity to be in an environment that encouraged freedom for theoretical design in healthcare. All employees at SCF are told that it is ok to think differently about the status quo, about what can be done to not only to make healthcare better, but to make it something entirely new.
As a patient, as a customer, and even as a provider, I invite you to consider—what do you want from your primary care experience?
Elia Cole
Osteopathic Medical Student - 4th Year (OMS IV)
College of Osteopathic Medicine
Pacific Northwest University of Health Sciences